A foot specialist’s guide to what has changed, what works, and when surgery is genuinely the right answer
Most people ignore their feet until walking becomes painful enough to change how they move through the day. By the time a patient sits down in my clinic and describes the grinding ache at the base of their big toe, or the bony bump that has made shoe shopping miserable for three years, or the crooked middle toes that catch on every sock they own, they have usually been managing symptoms for far longer than they should have.
That delay matters, because several of the most effective treatments for forefoot conditions work best when they are applied early. It also matters because the landscape of what is available has changed considerably over the past decade. Patients who received an inadequate answer five or ten years ago — “wear wider shoes and come back when it’s bad enough for surgery” — may not realise that better options now exist.
This article covers three common forefoot conditions: big toe arthritis, bunions, and hammer toes. For each, we look at what is actually happening in the joint or tissue, what conservative care can achieve, and what newer treatment approaches have added to the conversation.
Big toe arthritis: new treatment approaches beyond the traditional toolkit
Hallux rigidus — the clinical name for arthritis of the first metatarsophalangeal joint — is the most common arthritic condition of the foot. It affects the joint where the big toe meets the foot, progressively limiting the range of motion needed to walk, run, climb stairs, and push off the ground. In its early stages it often presents as stiffness in the morning and aching after activity. In later stages, the loss of dorsiflexion forces the body to compensate through the knee, hip and lower back, which is why patients with untreated hallux rigidus frequently develop secondary pain in places that seem unrelated.
The traditional approach to big toe arthritis treatment has centred on offloading: rigid-soled footwear, carbon fibre insoles, and cortisone injections to manage flare-ups. These remain useful first-line options, and for mild cases they can provide years of functional relief. But they address symptoms rather than the underlying joint deterioration, and their effectiveness diminishes as the condition progresses.
Among the newer treatment options for big toe arthritis that have gained meaningful clinical traction are viscosupplementation (hyaluronic acid injections into the joint), which some evidence suggests can reduce pain and improve range of motion in early-to-moderate disease, and platelet-rich plasma (PRP) therapy, which aims to leverage the body’s own growth factors to slow cartilage breakdown and reduce inflammation. Neither is a cure, and neither replaces the need for surgical intervention in advanced cases — but both have extended the conservative treatment window for many patients. More detail on the full spectrum of new treatment options for big toe arthritis is available for those who want to explore the evidence in depth.
On the surgical side, the field has also moved on. Cheilectomy — removing the dorsal bone spurs without fusing the joint — remains the gold standard for Grade I and II hallux rigidus when conservative care has failed. But for patients who want to preserve motion rather than accept arthrodesis (fusion), newer implant designs and cartilage restoration techniques have expanded what is possible at Grade III. The conversation about timing and surgical approach is worth having with a foot and ankle specialist before the disease forces the decision.
Bunion treatment: matching the intervention to the stage
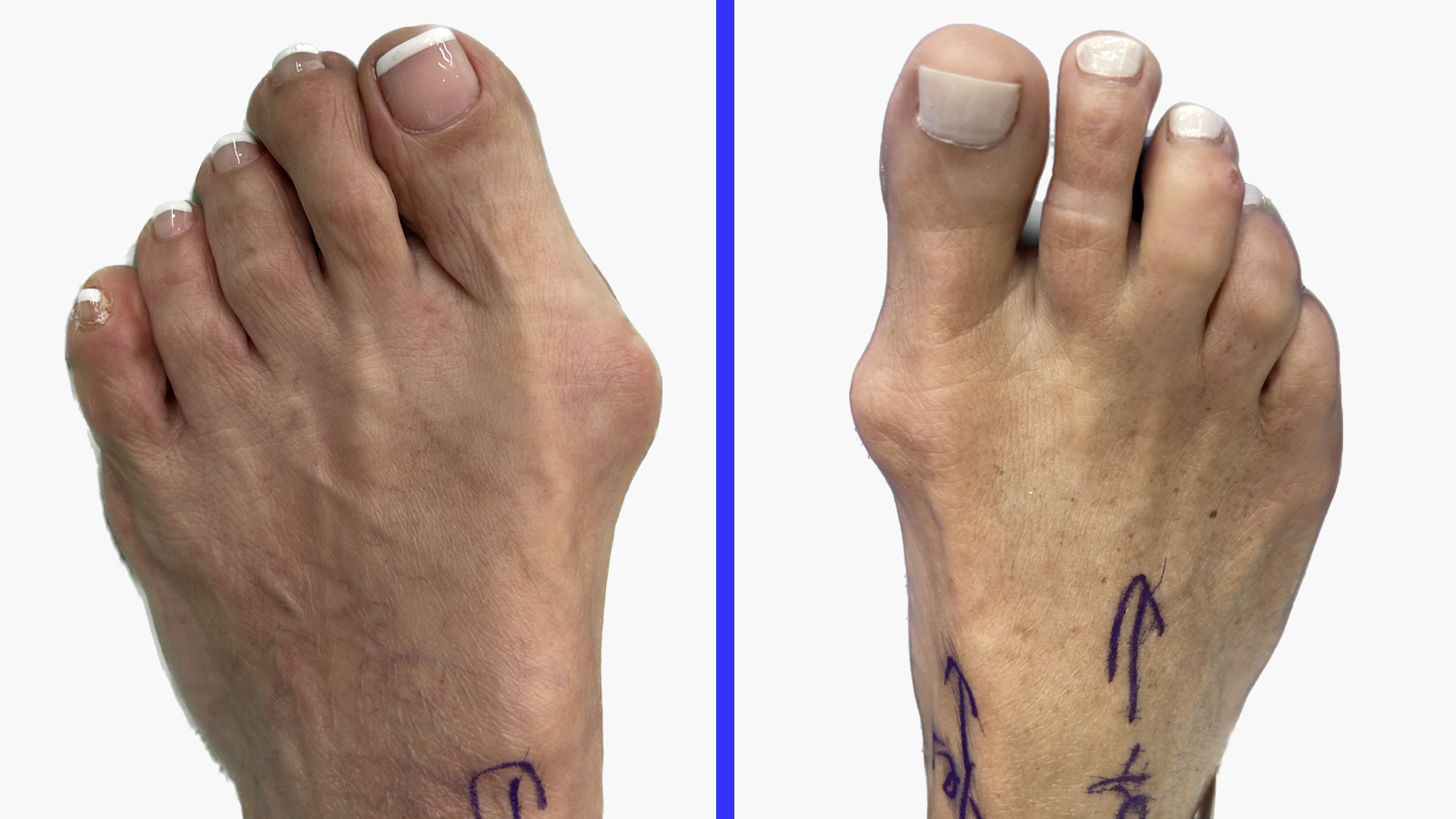
A bunion — hallux valgus — is a progressive structural deformity in which the big toe drifts toward the second toe and a bony prominence develops on the medial aspect of the foot. It is not simply a lump caused by tight shoes, though footwear can accelerate the process. The underlying driver is an instability in the first ray of the foot, often with a genetic component, that allows the first metatarsal to drift outward over time.
Treatment for bunions in 2026 is genuinely more individualised than it was a decade ago. Conservative bunions treatment — wider footwear, toe spacers, custom orthotics, activity modification, physiotherapy to strengthen the intrinsic muscles — remains the foundation of early management. For patients with mild to moderate deformity and no significant pain at rest, this approach can maintain function and delay progression for years.
When conservative bunion treatment has been exhausted and symptoms are limiting daily life, surgery becomes appropriate. What has changed in bunion surgery is the range of minimally invasive options now available. Percutaneous (keyhole) bunion correction techniques, which use small incisions and fluoroscopic guidance to realign the bone with minimal soft tissue disruption, have shown outcomes comparable to traditional open surgery in many studies, with faster recovery and less postoperative pain for suitable candidates. Not every bunion is a candidate for the minimally invasive approach — severity, bone quality and surgeon experience all factor in — but it is worth asking whether the option has been considered. A thorough overview of current bunion treatment approaches, from conservative management through to surgical planning, can help patients prepare for that conversation.
Tailor’s bunion — a bunionette on the fifth metatarsal head rather than the first — follows the same general treatment logic, though the anatomy differs and the surgical approach is distinct. Conservative management with offloading pads and appropriate footwear resolves many cases. When it does not, a metatarsal osteotomy to realign the fifth ray is typically effective with good long-term outcomes.
Hammer toe treatment: acting before the deformity becomes fixed
A hammer toe is a flexion deformity of the proximal interphalangeal joint of one of the lesser toes — most commonly the second. The toe buckles at the middle joint, creating a characteristic downward curve that can cause painful corns on the top of the toe from shoe pressure, and calluses on the ball of the foot from altered weight distribution.
The most important clinical distinction when evaluating hammer toe treatment is whether the deformity is flexible or rigid. A flexible hammer toe can be manually straightened — the joint still has passive range of motion. A rigid hammer toe has lost that mobility and is fixed in its deformed position. This distinction drives treatment almost entirely.
For a flexible deformity, treatment for hammer toe focuses on reversing the biomechanical drivers: custom orthotics to redistribute load, toe splints or straightening devices worn at rest, and occasionally a simple flexor tendon release procedure performed under local anaesthetic as a day-case procedure. Results at this stage are generally very good, recovery is swift, and the functional improvement can be dramatic.
For a rigid hammer toe, treatment options are more limited because the joint cannot be passively corrected. The surgical approach typically involves a proximal interphalangeal joint arthroplasty (removing a small section of bone to allow the toe to straighten) or arthrodesis (fusing the joint in a corrected position). Both procedures have a high rate of patient satisfaction when performed on the right candidate, though recovery takes longer than for flexible corrections.
The message for anyone dealing with hammer toes is straightforward: the earlier you seek assessment, the more options are available. A flexible deformity that could be managed conservatively or with a minor procedure can become a fixed deformity requiring more significant surgery within a few years if left unaddressed. Footwear that accommodates the toe, reduces pressure and prevents the deformity from progressing is not a glamorous intervention — but it works, and it buys time.
When to seek a specialist opinion
None of these conditions resolves on its own. Big toe arthritis progresses without intervention. Bunions drift further out of alignment over years. Flexible hammer toes become rigid ones. The shared lesson across all three is that early assessment does not commit you to early surgery — it gives you the full range of treatment choices, and the time to make them well.
If you have been managing forefoot pain with over-the-counter insoles and hope for longer than a few months, a formal clinical evaluation is worth your time. A specialist in foot and ankle conditions can confirm the diagnosis, stage the condition accurately, and lay out a treatment roadmap that is built around your activity goals and your timeline — not just the severity of the X-ray.